Depression is a clinically heterogeneous disorder, and as such can be treated through several approaches.1 A range of both pharmacological and psychological therapies make up today’s clinical repertoire of antidepressant treatments, while a number of alternative medicines, activities and techniques have also been claimed to offer some relief.2,3
According to NICE clinical guidance (CG90), it is recommended that patients with mild to moderate depressive symptoms should be offered either guided self-help, computerised cognitive behavioural therapy, a structured group physical activity programme, or a combination of these.4 However, for those patients who present with moderate or severe depression, a combination of both pharmacological intervention and a high-intensity psychological therapy should be prescribed.4
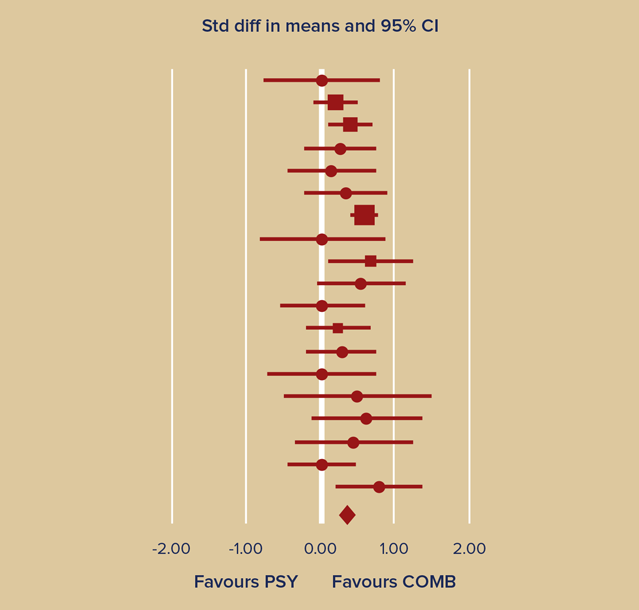
The research literature supports this recommendation. One meta-analysis of 19 randomised studies (figure 1) involving over 1800 patients with depression evaluated the difference in effect size between psychological therapy alone and a combination of both pharmacological and psychological treatment. It found a significant (P<0.001) difference in effect size between these two therapeutic approaches, with a combination strategy proving more efficacious.5
A number of alternative strategies have also been suggested to provide relief from depressive symptoms, including meditation, exercise, yoga, light therapy and St. John’s Wort.6-9 However, clinical research and experience focuses on psychotherapy and pharmacological treatments, and these remain the mainstay of clinical depression therapy.